What can care coordinators do within primary care?
Care coordinators are one of three additional roles under the umbrella of personalised care, with the aim of supporting people to improve their health and wellbeing, using a holistic approach and considering what matters to that individual.
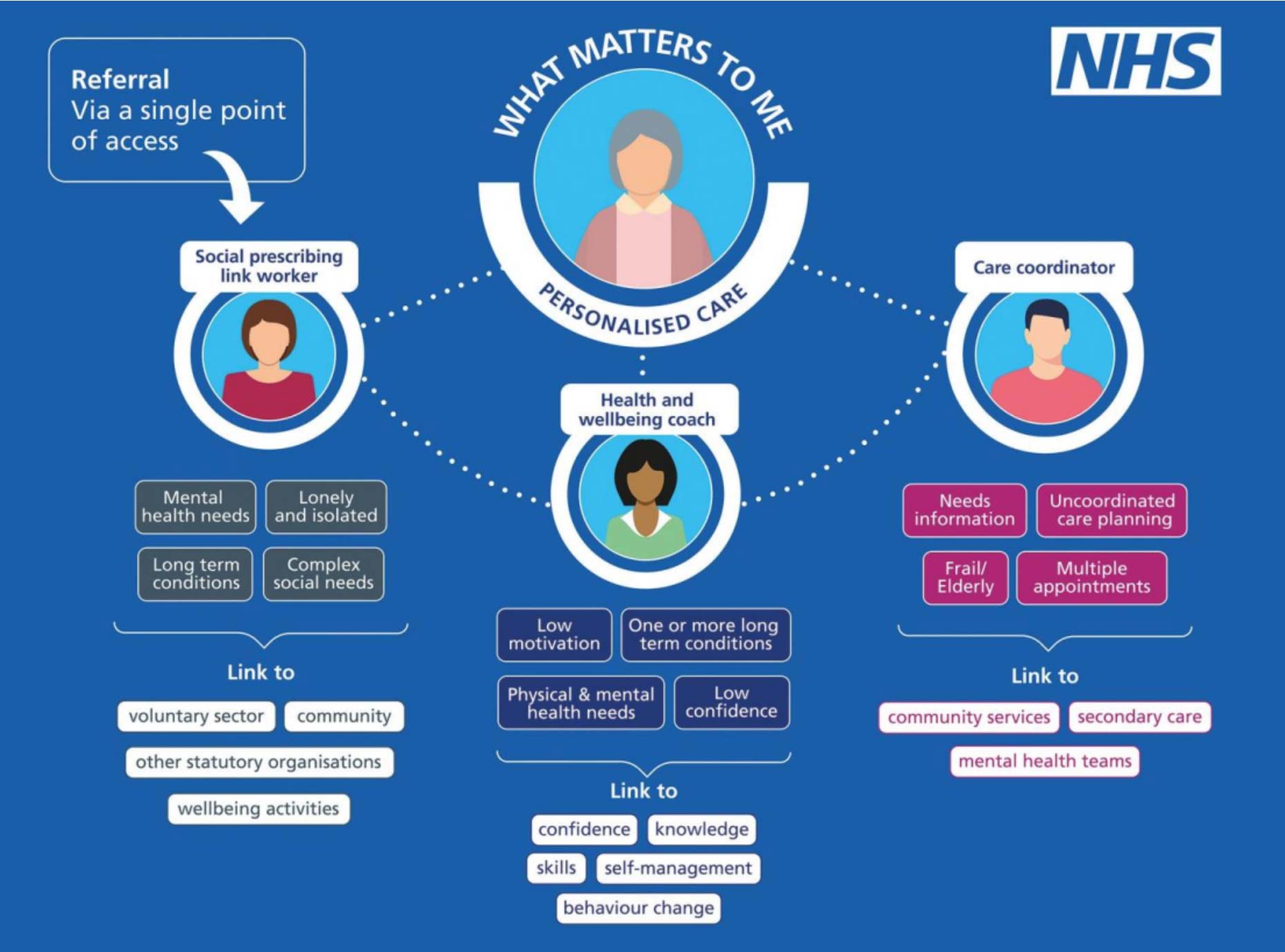
Given this broad remit the role of the care coordinator can be flexible to suit the PCN or population/community. Some of the roles care coordinators might undertake include:
- Proactive identification of people where support might be needed including those or are frail and/elderly and those with long term health conditions
- Provide co-ordination of care across health and social/care services
- Navigation of care and services and enabling patient choice
- Patient centred health and care planning, based on what matters to the person
- Support for care home patients (in some cases care coordinators may specialise in care home work)
- Support for palliative patients (again the role could be more specialist or might incorporate elements of this work)
- Reducing health inequalities
- Reducing the workload of GPs and other surgery staff to help ensure patients can access the right care at the right time
- Support with personal health budgets for those with complex needs
Training and supervision
Pre-requisites
There are no particular qualifications required to become a care coordinator and often this will come down to experience in relevant areas and the enthusiasm for the role. Further details can be found in the recruitment pack to the right of the page, under further resources.
Training pathway
The welcome pack, also seen on the right of the page, will provide some guidance to those new in role.
NHSE has developed a package of learning and support for care coordinators including webinars, online learning programme, regional training workshops and informal peer support. To access this please email england.supportedselfmanagement@nhs.net and tell them you’re a care coordinator, which PCN you’re part of and your contact details.
Further training is available via the personalised care institute. They have a list of accredited training providers who can provide training as deemed appropriate, for more information please click here.
Supervision
Having appropriate supervision within the practice and/or PCN is vital. These personalised care roles provide immense support for our patients, however they are often involved with complex and challenging patients. This is rewarding but does require support to ensure this doesn’t become a burden. A clinical supervisor is needed to provide day-to-day support as well as structured clinical supervision, often by way of a monthly review. Day-to-say support could be provided by the on call GP, but having named regular supervisor, often a GP lead is important. Please see induction section below for further information.
Induction
Please see the summary produced by Dr Olesya Atkinson to support social prescribers. Much of the guidance including the induction plan and supervision guidance is applicable to care coordinators. To access the summary please click here.
Peer support
Peer support is informally provided by NHSE on the email above in the training section. There is also a dedicated countywide peer support group for care coordinators, setup by the Gloucestershire Primary Care Training hub. Please contact us on glicb.pcwc@nhs.net if you would like to join.
Banding
4Welcome Pack
Related Case Study
-
A GP and care coordinator’s perspective (Reference: NHS futures)
and satisfying job I’ve ever done. I was motivated to take on this role, because I wanted to help individuals and families impacted by a life-limiting condition based on my own personal family experience.

